Cardiac Cath Lab Tech: The High-Adrenaline Imaging Career
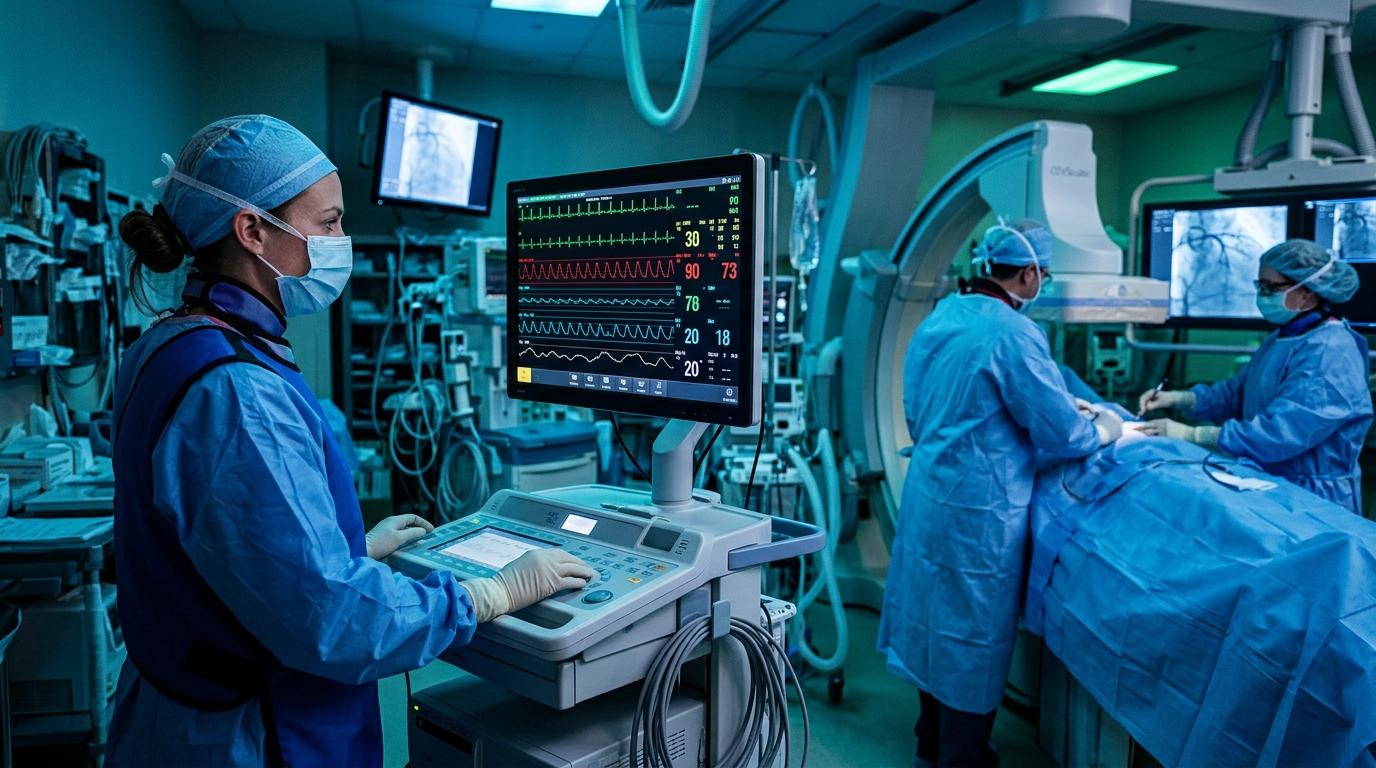
I'll never forget when Sarah, a cath lab tech I coached, described her job: "It's like regular radiology, except every day feels urgent, you're operating million-dollar equipment, and the cardiologist is making real-time decisions based on your images. People's lives depend on getting this right."
Then she paused: "And I absolutely love it."
The cardiac catheterization lab is one of the most dynamic and high-stakes specialties in medical imaging. It's not for everyone. The pace, stakes, and skill set all extend beyond traditional radiology training. But for someone who thrives in complex clinical situations and wants immediate patient impact, it's genuinely unique.
I've coached many radiology professionals who've transitioned into cath lab or are considering it. I want to walk you through what this work actually is, what makes it different, and whether it might be right for your career.
What Actually Happens In A Cath Lab
Here's the thing about cath lab that most general radiographers don't fully understand until they work there: it's not a typical imaging department. It's more like an operating room that happens to have advanced imaging equipment.
A cardiac catheterization lab is where cardiologists perform diagnostic and interventional procedures on the heart and coronary arteries. This might include angiography (injecting contrast to visualize blood vessels), placing stents to open blocked arteries, performing balloon angioplasty, inserting devices like pacemakers, or managing other cardiac interventions. The procedures range from diagnostic (just visualizing the anatomy) to highly complex interventional work where the cardiologist is literally changing the patient's cardiac physiology in real-time.
As a cath lab technologist, you operate the fluoroscopy equipment that lets the cardiologist see what they're doing. You control the C-arm (the imaging equipment that rotates around the patient), adjust angles, manage exposure, acquire images, and time contrast injections perfectly.
But you're also part of a high-functioning team—nurses, cardiologist, possibly a perfusionist—that works seamlessly while managing critical, often unstable patients.
Marcus, another tech I coached, put it this way: "In diagnostic radiography, you set up an image and the patient leaves. In cath lab, you're providing live guidance. The cardiologist is looking at your images in real-time and making decisions based on them. Image quality, anticipating views, catching details—it all directly affects the procedure. You can't be passive."
That's the core difference. You're not just producing images. You're a key part of the clinical team.
The Skills You Need (And You'll Develop)
Working as a cath lab technologist requires some baseline imaging knowledge. Most cath lab positions want you to be an ARRT-certified radiologic technologist. Some want specific background in interventional procedures or cardiovascular imaging, though many facilities will train someone who's motivated and has solid foundational radiology skills.
But the real skill set for cath lab goes beyond what you learn in traditional RT school:
Fluoroscopy expertise. You need to be genuinely good with fluoroscopy systems. Not just knowing how to operate them, but understanding the equipment deeply. Image quality, exposure management, troubleshooting problems, optimizing images for specific cardiac structures. This is the bread and butter of cath lab work, and it takes time to master.
Anatomy knowledge. You need to know cardiac anatomy inside and out—coronary arteries, chambers, valves, conduction system—in the angles where cardiologists view them. Unlike general radiology where you can reference guides, in cath lab you work at speed and must immediately know which view shows specific structures.
Procedure knowledge. Understanding what procedure is happening, what the cardiologist is trying to accomplish, and what views they'll need develops over time and with experience. Good cath lab techs can anticipate the next view, position equipment before being asked, and predict potential problems.
Communication skills. You work directly with the cardiologist throughout the procedure, not like diagnostic imaging where they review later. You're in constant conversation, responding to requests, flagging concerns about quality or positioning. You need to be clear and collaborative under pressure.
Technical problem-solving. Cath lab equipment is complex. Things go wrong—equipment malfunctions, imaging issues, patient positioning challenges. You need to be able to troubleshoot quickly and either fix it or communicate the problem to the right person immediately. Downtime costs money and puts patients at risk.
Attention to detail. Contrast timing has to be perfect. Patient positioning matters enormously. Your documentation of procedures needs to be accurate. You're working with equipment that produces radiation and you need to manage exposure carefully. Mistakes in this environment can have real consequences, so there's very little room for carelessness.
What The Day-To-Day Actually Feels Like
Here's what a typical shift feels like, based on conversations with techs I've coached.
You arrive and review the schedule: maybe four cases—a diagnostic cath (30-40 minutes), two interventional cases (60-90 minutes each), one pacemaker implant (45 minutes to three hours depending on complexity).
You prep the equipment, test the fluoroscopy system, make sure everything's working properly. You're thinking through angles and views for the cases. You know cardiac anatomy well enough that you're already visualizing the procedures.
The first patient arrives. You position them, establish access, start the diagnostic cath. The cardiologist guides the catheter while you provide real-time images, adjust the C-arm, and anticipate the next view. A steady stream of requests comes: "Left anterior view." "Cranial." "Give me caudal." You make minute adjustments.
One case turns into an intervention. What was diagnostic becomes a stent placement. Complexity ramps up. The cardiologist's focus intensifies. The nursing team's pace increases. Adrenaline is higher.
You manage radiation exposure while protecting the patient and team. You watch vitals, communicate with the team.
Cases move fast with brief breaks between. Documentation, equipment maintenance, prep for the next case happens in minutes.
By shift's end, you're mentally fatigued from eight hours of focus, quick decisions, and complex clinical situations.
Jessica, another tech: "It's the most engaging work I've done. There's no autopilot. Every case is different, every cardiologist has different preferences, every patient presents differently. I'm completely present for eight hours. I never feel like I wasted my time."
What The Training Timeline Looks Like
If you're a general radiographer with solid ARRT certification and want to transition into cath lab, the timeline varies significantly by facility.
Some larger hospitals have formal cath lab training programs. You might spend four to six weeks in a structured program, shadowing, learning the specific equipment, understanding procedures, developing advanced fluoroscopy skills, and building cardiac anatomy knowledge. During this time, you gradually move from observing to operating equipment with supervision to independent work.
Smaller facilities might have less formal programs. You could be trained on the job over a few months, mentored by experienced cath lab techs.
Most importantly, you need to be genuinely willing to learn. The best cath lab techs are deeply invested in understanding the procedures, the anatomy, the equipment. They read about cardiac interventions. They ask questions. They pay attention to how things connect.
There's also continuing education specific to cath lab. ARRT offers a Cardiac Interventional Radiography certification, which many techs pursue after they've worked in the specialty for a bit and want to formalize their expertise.
Is Cath Lab Right For You?
Not every good radiographer should be a cath lab tech. And not every cath lab tech would be happy doing general radiography.
Cath lab is right for you if:
You thrive in fast-paced, high-stakes environments. If you get bored with routine and get energized by intensity, this specialty is a fit.
You want immediate patient impact. You're not waiting for a radiologist to review images later. You're in the room watching the procedure, seeing the direct results of your technical skill.
You're genuinely interested in anatomy and procedures. This isn't something you can just technically execute. You need to care about the "why" of what's happening.
You want to be part of a clinical team. You're not a solo operator. You're collaborating constantly with cardiologists, nurses, and other specialists.
You're willing to be on-call or have variable scheduling. Cardiac emergencies don't happen on predictable schedules. Many cath labs have on-call requirements, especially at hospitals that do emergency cases.
You're someone who grows through challenge. The learning curve is steeper than general radiography. If you like professional growth and developing expertise, that's compelling.
Cath lab is probably not right for you if:
You want a calm, predictable workday, or you prefer working independently. You're not interested in deepening anatomy and procedural knowledge. Or you're looking for the easiest path to higher income without additional training and responsibility.
The Career Path In Cath Lab
Cath lab opens multiple pathways. Some techs stay and become deeply expert specialists that cardiologists request. Others use it as a stepping stone into neurointerventional, vascular interventional, or other specialty imaging. Some move into management, supervision, or education. Others transition into clinical roles like nursing or interventional cardiology.
The specialty is deep enough for a full career or technical and clinical enough to open other doors.
Salary-wise, cath lab techs typically earn 10-15% more than general radiographers, with experienced techs commanding premium compensation in urban markets or larger hospitals.
Making The Transition
If you're interested in moving into cath lab, here's what I'd recommend:
First, get exposure. See if you can observe a cath lab in action. Talk to cath lab techs about their work. Understand what the job actually entails before committing to training.
Second, be a strong general radiographer. Facilities want people with solid foundational imaging skills. Competence in general radiography makes the transition to cath lab much smoother.
Third, look for dedicated training programs. Training quality matters. You don't want to be learning on the fly with inadequate mentorship. Facilities with formal programs invest in their techs.
Fourth, invest in the specialty. Read about cardiac interventions. Learn the anatomy deeply. Show up to your training program ready to engage meaningfully, not just technically checking boxes.
Cath lab isn't for everyone. But for radiography professionals who want to work at the intersection of advanced technology, clinical complexity, and immediate patient impact, it's genuinely one of the most rewarding specialties in imaging. You'll be challenged, engaged, and part of something meaningful every single day.
Related Articles
Breast Imaging Specialist: Why Mammography Techs Are in Such High Demand
April 16, 2026

The ROI of Investing in Rad Tech Continuing Education
April 16, 2026

Managing a Multi-Generational Radiology Department
April 16, 2026

Credentialing and Compliance: A Hiring Manager's Checklist for New Rad Tech Hires
April 15, 2026